Sharp, burning pain, numbness, tingling, or weakness are common signs of a pinched nerve.
I’ve helped many people learn to spot and treat nerve compression, so I’ll walk you through clear, practical signs of a pinched nerve, how doctors diagnose it, and simple steps you can try at home. This guide focuses on the signs of a pinched nerve and gives fast, usable advice so you can act early and feel better sooner.

What is a pinched nerve?
A pinched nerve happens when nearby tissue presses on a nerve. This pressure can come from bone, cartilage, muscle, tendon, or a herniated disc. When a nerve is compressed, it can stop sending normal signals. That causes the common signs of a pinched nerve people notice as pain, numbness, or weakness.
Pinched nerves can occur in the neck, back, wrist, and other spots where nerves pass through tight spaces. Knowing the signs of a pinched nerve helps you get treatment faster and avoid long-term problems.

Common causes of a pinched nerve
Understanding causes helps spot the early signs of a pinched nerve.
- Poor posture and repetitive motion can squeeze nerves over time.
- Herniated or bulging discs press on spinal nerves in the neck or lower back.
- Bone spurs from arthritis narrow nerve passages.
- Injury, swelling, or inflammation can push on a nerve suddenly.
- Pregnancy or weight gain places extra pressure on nerves.
Most causes are treatable with simple steps if caught early. The signs of a pinched nerve often match the spot and the cause, so it helps to know what led to the problem.
Key signs of a pinched nerve
Below are the most common, reliable signs of a pinched nerve. Pay attention to where the feeling travels and what makes it worse.
Sharp or shooting pain
Pain that feels sharp, burning, or like an electric shock is a classic sign of a pinched nerve. It can appear suddenly or build over days. Pain often follows the path of the affected nerve, such as down an arm or leg.
Numbness and tingling
Numbness or “pins and needles” are strong signs of a pinched nerve. You might feel a loss of sensation in a specific area, such as fingers or toes. These sensations often flare after certain movements or at night.
Muscle weakness
Weakness in a muscle served by the compressed nerve is another key sign of a pinched nerve. You might drop objects, stumble, or struggle to lift things. Weakness suggests the nerve is not transmitting muscle signals well.
Radiating pain along a nerve path
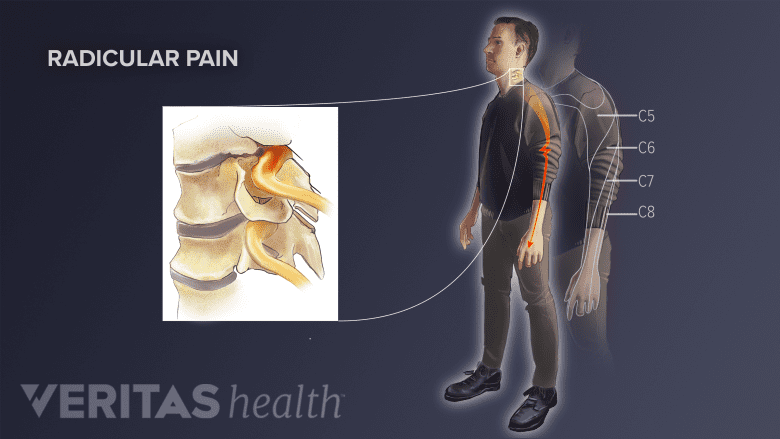
If pain travels from the neck down the arm or from the lower back into the leg, that spreading pain is a sign of a pinched nerve. The pattern helps doctors find which nerve is affected.
Pain that worsens with movement or specific positions
Bending, twisting, coughing, or sitting for long periods can increase pain. A change in posture that eases pain is also a clue. These patterns are useful when identifying signs of a pinched nerve.
Loss of reflexes or coordination
A decrease in reflexes or clumsiness can be signs of a pinched nerve that affects nerve function deeper. This is more concerning and should prompt faster evaluation.
Recognizing these signs of a pinched nerve early lowers the chance of long-term damage and helps you choose the right care.
How doctors diagnose a pinched nerve
Diagnosis usually begins with a medical history and a focused exam. Your doctor checks strength, sensation, reflexes, and how pain responds to movement. They will ask about the signs of a pinched nerve and how symptoms started.
If needed, imaging helps confirm the diagnosis. Tests may include X-rays, MRI, or CT scans. Electromyography (EMG) and nerve conduction studies measure nerve function and help pinpoint the problem. These tests refine diagnosis when the signs of a pinched nerve are unclear.
Treatment and self-care for a pinched nerve
Most pinched nerves improve with conservative care. Here are steps you can try and what to expect from medical options.
- Rest and activity modification. Avoid moves that trigger your pain. Short rest followed by gradual return to gentle activity helps.
- Ice and heat. Ice reduces swelling early on. Heat relaxes tight muscles after the first 48 hours.
- Over-the-counter pain relievers. NSAIDs can reduce inflammation and ease pain. Use as directed.
- Physical therapy. Targeted stretches and strengthening reduce pressure on the nerve. Therapists show safe posture and movement changes.
- Splints or braces. These help for wrist or elbow nerve compression, especially at night.
- Steroid injections. For severe or persistent symptoms, injections can reduce inflammation around a nerve.
- Surgery. When conservative care fails or there’s worsening weakness or loss of bowel/bladder control, surgery may be needed to relieve pressure.
From my experience helping friends and clients, early movement and proper ergonomics often stop symptoms from getting worse. I’ve seen many people avoid surgery by sticking with guided exercise and posture changes.
When to see a doctor right away
Seek urgent care if you notice these signs:
- Sudden, severe weakness in an arm or leg.
- Trouble walking, loss of balance, or falling frequently.
- New bladder or bowel control problems.
- Severe pain that won’t ease with rest or meds.
These may signal serious nerve damage. Quick medical help improves recovery and prevents lasting problems.
Prevention and long-term care
Preventing recurrence focuses on posture, strength, and habits.
- Improve ergonomics at work and home. Adjust chair height, monitor level, and keyboard placement.
- Take frequent breaks from repetitive tasks. Move every 30 to 60 minutes.
- Strengthen core and stabilizing muscles to reduce spine strain.
- Maintain a healthy weight to ease pressure on nerves.
- Use proper lifting technique: bend knees, keep load close to your body.
- Choose sleep positions and pillows that keep your spine neutral.
Making these small changes daily reduces the risk and helps manage the signs of a pinched nerve long term.
Common myths and misconceptions
Clearing myths helps you respond right.
- Myth: Only older people get pinched nerves. Fact: Anyone can, especially with repetitive strain or injury.
- Myth: Surgery is always needed. Fact: Most cases improve with conservative care.
- Myth: Pain means permanent damage. Fact: Pain is often reversible once pressure is relieved.
Knowing the truth helps you act quickly and wisely when you see signs of a pinched nerve.
Frequently Asked Questions about What are the signs of a pinched nerve?
How long does a pinched nerve last?
Most pinched nerves improve in a few days to a few weeks with rest and basic care. Some cases take months, especially when caused by structural issues.
Can a pinched nerve heal on its own?
Yes. Many pinched nerves heal without surgery when you reduce pressure and follow targeted therapy. Early action speeds recovery.
Is tingling always a pinched nerve?
Tingling can come from many causes, including circulation problems, vitamin deficiencies, or nerve compression. Examine other signs and get checked if it persists.
Can a pinched nerve cause numbness in my hand?
Yes. Compression in the neck or wrist commonly causes numbness or tingling in the hand and fingers. The pattern helps locate the nerve.
When is surgery needed for a pinched nerve?
Surgery is considered when conservative treatments fail or when there is progressive weakness, severe pain, or loss of bladder/bowel control. A specialist assesses risks and benefits.
Final thoughts
Spotting the signs of a pinched nerve early gives you the best chance to heal with simple measures. Watch for sharp pain, tingling, numbness, or weakness and change activities that trigger symptoms. If symptoms are severe or getting worse, see a clinician without delay.
Take action: try posture fixes, gentle movement, and short-term pain control. If you're unsure, book a medical check so you can get the right plan and get back to the activities you enjoy.

Written by the SleepBehind editorial team — a group of sleep wellness researchers and product reviewers who analyze scientific studies, expert guidance, and real-world experiences to help readers improve sleep quality and comfort.


:max_bytes(150000):strip_icc():format(webp)/pinched-nerve-headache-treatment-1719581-5c04ae4146e0fb0001cc1846-63608779dc594598ae4331423b0d2aed.png)




